This year, pharmacy director Jacarre Shelton had a plan for shutting down if 25-bed Adventist Health Clear Lake hospital were to order evacuation because of a nearby wildfire.
The plan—based on an earlier experience when the hospital evacuated—has not had to be put into practice this summer fire season, he said.
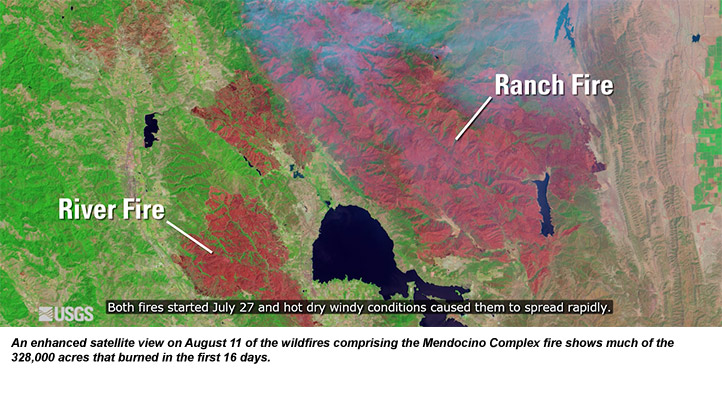
Instead, the critical access hospital was on the receiving end when California’s largest wildfire in history, the Mendocino Complex fire, led to evacuation of 25-bed Sutter Lakeside Hospital, which is in a community on the northwest shore of Clear Lake.
“So many levels of stress go on during the fire,” said Shelton, who has been pharmacy director through 4 consecutive years of major wildfires in the areas surrounding the hospital’s community, on the southeast end of the lake.
Not only can a wildfire result in a sudden influx of inpatients, it can lead to a rush of ambulatory patients in the emergency department who must evacuate their homes but could not obtain their medications at their usual community pharmacy, he said. That’s in addition to the residents who tend to use the emergency department as their preferred site for primary care when smoke in the air makes breathing difficult. Such visits, he noted, result in the pharmacy supplying a lot of inhalation medications to the emergency department.
All the while, employees with homes near the wildfire are working while receiving electronic alerts, listening to word-of-mouth news, and rightfully worrying about their family, animals, and possessions, Shelton said.
The pair of wildfires that the California Department of Forestry and Fire Protection soon renamed the Mendocino Complex started on July 27 in the county west of the Clear Lake communities.
On day 2, Saturday, the department announced evacuation of portions of Lakeport. At 6:54 p.m., Sutter Health tweeted that its Lakeside Hospital, in Lakeport, was in the mandatory evacuation zone. A follow-up tweet reported the transfer of 13 patients “to other nearby community hospitals.”
On Sunday, according to additional tweets, Sutter Health reopened in the morning but discharged or transferred 1 inpatient and 7 emergency room patients to area hospitals and was evacuated before evening.
Adventist Health St. Helena, in the county south of Clear Lake, received some of the patients, said pharmacy director Alan Ahmad.
On a normal Saturday, he said, the inpatient pharmacy at the 144-bed hospital closes at 6:30 p.m.
“But we got the heads-up from the nursing supervisor that we’d be receiving patients in the evening,” Ahmad said.
He had a pharmacist come in at 6:30 p.m. to handle the inpatients arriving from Lakeport. A pharmacy technician volunteered to stay in support of that pharmacist.
“I was in Sacramento,” Ahmad said. “But I drove back to Napa and arrived here at 9 p.m., and we started seeing the orders come through.”
By about 1:30 a.m., all the medication orders had been processed and initial doses delivered to the patient care areas, he said.
Shelton said that obtaining information about the medications being taken by the newly arrived patients proved to be “kind of a daunting task.”
Because the patients’ hospital had closed down, he said, the nurses at Adventist Health Clear Lake had to call other hospitals in the Sutter system and ask personnel there to view the electronic medical records and provide the needed information.
Obtaining pharmacy supplies during the recent wildfire was not a problem, Shelton said, although the delivery driver had to use an alternative route to reach the hospital. Anything needed in a quick time frame was obtained from Ahmad’s pharmacy.
In St. Helena, Ahmad said, the pharmacy team worked to anticipate needs. Personnel viewed the medication profiles of inpatients who were expected to be transferred from the smaller sister hospital and estimated the need for additional i.v. fluids and critical medications.
The pharmacy technician who orders supplies for the St. Helena inpatient pharmacy did so from her house, which was near an evacuation zone, Ahmad said. She arranged for other staff members to be able to order supplies in case she had to evacuate.
Shelton said he was at home, in Berkeley, the most recent time his hospital was evacuated.
“The [other] pharmacist called me and said, ‘They told us we have to get out in 15 minutes. So, what do you want us to grab?’” he recalled.
Based on that experience, Shelton said, the staff now has an in-case-of-evacuation checklist. There is a list of the medications—the most expensive products—to remove and store appropriately offsite. There is a reminder to print out the narcotic inventory and photocopy each patient care unit’s narcotic sheet. There is a folder that has the lists of the items in all the pharmacy’s kits.
Ahmad, who directs a 20-person department and lives in Napa, 4 communities south of St. Helena, said “keeping your cool” is important for a leader during a situation like a wildfire. So are respecting personal situations and ensuring that everyone understands why certain things are being done.
“In the past year, when the fire was getting close, those staff that live close-by, I let them go home,” he said.
To assist him, Ahmad said, he relied on those staff members who drove to the hospital from points south.
As for his own situation, he prepared his family to function without him during the wildfire.
Shelton said he slept 2 nights in the pharmacy during the previous wildfire that threatened the community of Clearlake.
“It was just easier for me to stay” than endure more than 4 hours of slow traffic on the drive home, he said. “So I got an air mattress from the local Walmart.”
When interviewed, Shelton said the hospital was still using large fans indoors to remove the smoke that remains a prominent force in Clearlake.
[This news story appears in the November 15, 2018, issue of AJHP.]